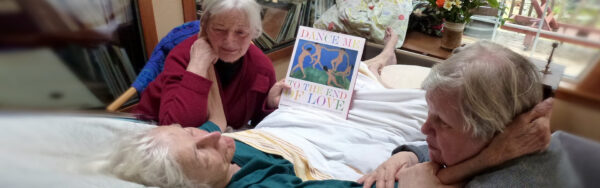
Providing optimal care at end-of-life is essential. However, it becomes near-to-impossible when end-of-life care is not discussed until end-of-life.
The need to provide excellent end-of-life care for all people is acknowledged worldwide. The issues arise in knowing how to prepare for optimal end-of-life care.
Fortunately, the recommendations in the Framework on Palliative Care in Canada2 in part, address the barriers mentioned in the research. The recommendations of Harasym et al, (2020) from their research align well with the principles of palliative care and include:
- Using standardized tools to help address understanding of pain with dementia
- Assessing routinely to help prevent crisis
- Engaging spiritual care providers who also had some medical knowledge would help to support family
- Improving staffing ratios to ensure caregivers were available to provide more intensive end-of-life care
These strategies will help the care team to support the person and family in providing optimal care at end-of-life. However, it becomes very difficult when end-of-life care is not discussed until end-of-life.
Preparing for optimal end-of-life care is what a palliative approach is about
Integrating a palliative approach to care early in the person’s illness, possibly when they are still living in the community, enables appropriate information sharing with the person and family about the illness and helps them to understand what to expect. With a palliative approach, information sharing and serious illness conversations can be approached gently over time, instead of in urgent situations when the person is at end-of-life.
Integrating a palliative approach also means that palliative care is not the sole responsibility of the specialist, in this case, the physician. The entire care team—PSWs, nurses, socials workers, care directors, and so on, are involved in supporting the person and family through the person’s illness and death. Together with the family and community, the team gathers information about the person, their beliefs, values and goals of care. With this knowledge the care team is better able to meet the person’s physical, spiritual, emotional and mental health needs at end-of-life. And with a palliative approach, care planning conversations that occur long before end-of-life in both formal and informal ways, can help decrease fears and help prepare the person and family for future changes.
Educating all care providers
One thing that 2020 has made apparent is that health care is woefully unprepared to support greater numbers of people living and dying with life-limiting illness. The predicted number of Canadians with dementia who will need care in the year 2030 is astounding – an increase of 66% to an estimate of 937,000 people.
It is possible to prevent or address the barriers mentioned by Harasym et al (2020) and provide optimal end-of-life care—by educating all members of the care team, including physicians, in providing basic palliative care and integrating a palliative approach. To meet the care needs of people in the coming years, all members of the care team will need to be able to integrate a palliative approach now. Today. Tomorrow and next month and next year.
This means educating all caregivers to be confident and competent in preparing to care, opening doors to serious illness conversations, managing physical comfort, ways of responding to serious illness questions from the person and family, and palliative care best practices in communication. With this training, the health care team will be able to provide optimal end-of-life care for people dying in the coming years.
1 Harasym P, Brisbin S, Afzaal M, et al. Barriers and facilitators to optimal supportive end-of-life palliative care in long-term care facilities: a qualitative descriptive study of community-based and specialist palliative care physicians’ experiences, perceptions and perspectives. BMJ Open 2020;10:e037466. doi:10.1136/bmjopen-2020-037466
2 Health Canada, Framework on Palliative Care (2018) https://www.canada.ca/en/health-canada/services/health-care-system/reports-publications/palliative-care/framework-palliative-care-canada.html










